There are many reasons why patients experience swelling of the feet. It is rather common and may be a side effect of pregnancy or from sitting and standing for most of the day. Gravity could also play a role in the development of swollen feet. It is known that the weight of blood volume in our bodies is exerted on the veins in the legs and feet. The veins may not work as efficiently during the aging process, and this could make the blood flow backward causing swollen feet. Relief may be found when obese patients lose weight, and it may help to engage in compression therapy by wearing compression socks, stockings, or athletic sleeves. This method can release pressure on the feet and ankles which may help to reduce existing swelling. There are patients who have controlled their swollen feet by implementing healthy lifestyle changes. These can consist of reducing salt intake, incorporating a gentle exercise regime into the daily routine, and drinking plenty of fresh water. Swollen feet may be a temporary condition that affects people who travel via airplane or automobile, so it is beneficial to walk as frequently as possible even though it can be difficult. Swelling of the feet can also be indicative of other health issues so it is important to pay attention to any type of chest pain, mental confusion, dizziness, or fever. If you consistently have swollen feet, it is strongly suggested that you consult with a podiatrist who can help determine the cause and how to effectively treat it.
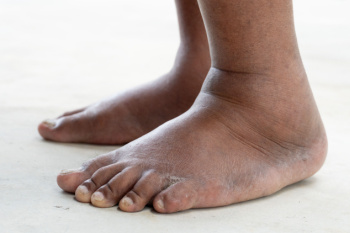
Swollen feet, a condition known as edema, is common among people with diabetes. Edema occurs when fluid builds up in the tissues, leading to puffiness, especially in the feet, ankles, and legs. Diabetes can contribute to edema due to poor circulation, nerve damage, or kidney problems, all of which make it harder for the body to regulate fluid properly. Symptoms of swollen feet include visible puffiness, tight or shiny skin, and discomfort. If left untreated, swelling can lead to complications, including infections or ulcers, especially in diabetic patients with reduced sensation in their feet. Treatment for edema typically involves elevating the feet, wearing compression socks, managing blood sugar levels, and limiting salt intake. In some cases, a podiatrist may recommend specific exercises or custom footwear to alleviate pressure. If you are experiencing swollen feet, it is suggested you schedule an appointment to see a podiatrist. Early intervention can prevent further complications and provide effective relief.
Swollen feet can be a sign of an underlying condition. If you have any concerns, contact one of our podiatrists of Jill Einhorn, DPM and James Einhorn, DPM. Our doctors can provide the care you need to keep you pain-free and on your feet.
Swollen feet are a common ailment among pregnant women and people who stand or sit for extended periods. Aging may increase the possibility of swollen feet and patients who are obese often notice when their feet are swelling too. There may be medical reasons why swollen feet occur:
Swollen feet can also be caused by bone and tendon conditions, including fractures, arthritis, and tendinitis. Additionally, there may be skin and toenail conditions and an infection may cause the feet to swell. Patients who take medicine to treat high blood pressure may be prone to getting swollen feet.
Many patients elevate their feet to help relieve the swelling and this is generally a temporary remedy. When a podiatrist is consulted the reason behind the swelling can be uncovered and subsequently treated.
If you have any questions please contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

Foot stress fractures are small cracks in the bones of the foot, often resulting from repetitive stress or overuse. Common causes include high-impact activities, sudden increases in exercise intensity, and inadequate footwear. Symptoms typically include localized tenderness, pain, and weakness in the affected area, especially during physical activity or when putting weight on the foot. Swelling and bruising may also occur. Treatment for stress fractures focuses on rest and immobilization. A podiatrist may recommend using a walking boot or crutches to reduce pressure on the foot, along with anti-inflammatory medications to alleviate pain. Gradual rehabilitation exercises can also help restore strength and flexibility. If you suspect you have a foot stress fracture, it is suggested that you consult a podiatrist. They can provide an accurate diagnosis and develop a tailored treatment plan to promote healing and prevent future injuries.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact one of our podiatrists from Jill Einhorn, DPM and James Einhorn, DPM. Our doctors can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions please contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
Many foot diseases and conditions become more serious and common among the elderly. Some of these conditions include diabetic ulcers, ingrown toenails, fungus, arthritis, corns, and calluses. Unfortunately, it may be harder for older adults to take care of their own feet, but there are some precautions they can take in order to avoid any serious conditions.
Dry, cracked heels tend to be a common problem for older people. In order to avoid this, you should always keep your feet clean and well moisturized. Special feet moisturizers should be used as average lotions might not provide enough moisture for dry and cracked heels. Daily foot inspections are crucial for the elderly to detect any irregularities in their earliest stages. During the aging process, blood circulation tends to slow down causing older people to not feel their feet as well as they used to. This often results in foot problems going unnoticed.
Fungal and bacterial conditions thrive on elderly feet because older adults are less likely to keep their feet clean and dry; this makes it easier for bacteria to take hold in their dry, cracked skin. Elderly people should be sure to thoroughly dry their feet, especially in between the toes, after bathing. This will help them avoid developing any fungal infections. Additionally, clean cotton socks should be worn after the feet are dried.
Cutting toenails straight across will help prevent ingrown toenails. When toenails are cut too lose, the nail might break through the skin resulting in an ingrown nail. Clippers should be used to cut the nails in order to make the cut even.
Elderly people who have diabetes are at risk of developing serious foot problems that may lead to amputation. Ulcers that are left untreated can lead to gangrene. Dry and cracked feet, fungus, and untended cuts under the nails may also lead to infections.
Fortunately, Medicare covers many different types of services for foot care. Elderly people with any of these foot conditions should seek the help of a podiatrist and perform daily foot inspections in order to ensure that they have healthy feet.
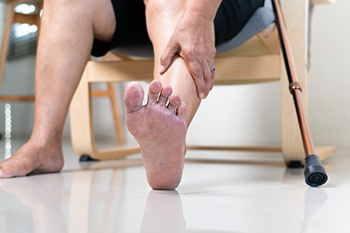
In older adults, foot and ankle pain is common. Pain originating in the feet often includes arthritis, bunions, and plantar fasciitis, which develop due to joint wear, inflammation, or tissue strain. Conversely, pain can also start outside the feet from nerve compression in the spine or hip arthritis, which can radiate down to the feet and cause discomfort. Aging naturally changes foot structure. Fat pads on the soles are thin, making feet more vulnerable to pressure, skin becomes drier and less elastic, and ligaments may stretch, causing flat feet or instability. Treatment often includes supportive, well-fitted shoes and custom orthotics to reduce strain. In more severe cases, injections, like corticosteroids, reduce inflammation. Surgery may be necessary to correct structural issues or relieve persistent pain. If you are elderly and experience foot or ankle pain, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
Proper foot care is something many older adults forget to consider. If you have any concerns about your feet and ankles, contact one of our podiatrists from Jill Einhorn, DPM and James Einhorn, DPM. Our doctors can provide the care you need to keep you pain-free and on your feet.
The Elderly and Their Feet
As we age we start to notice many changes in our body, but the elder population may not notice them right away. Medical conditions may prevent the elderly to take notice of their foot health right away. Poor vision is a lead contributor to not taking action for the elderly.
Common Conditions
Susceptible Infections
Diabetes and poor circulation can cause general loss of sensitivity over the years, turning a simple cut into a serious issue.
If you have any questions, please feel free to contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
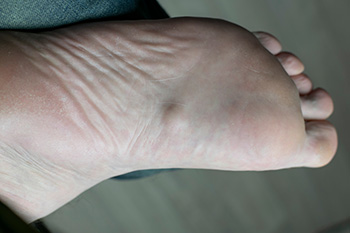
A plantar fibroma is a benign tumor that develops in the plantar fascia, the thick band of tissue running along the bottom of the foot. Typically found in the arch, it appears as a firm lump that may cause discomfort during walking or standing. Diagnosing a plantar fibroma involves a thorough medical history and physical examination, where a podiatrist will assess the lump's size, location, and texture. Imaging studies such as ultrasound or MRI scans may be employed to confirm the diagnosis and rule out other conditions. The exact causes of plantar fibromas remain unclear, though factors such as genetics, trauma, and certain medical conditions may contribute to their development. Having a plantar fibroma can be uncomfortable. If you have developed this condition, it is suggested that you consult a podiatrist who can offer you relief options.
A plantar fibroma may disrupt your daily activities. If you have any concerns, contact one of our podiatrists of Jill Einhorn, DPM and James Einhorn, DPM. Our doctors can provide the care you need to keep you pain-free and on your feet.
Plantar Fibroma
A plantar fibroma is a fibrous knot in the arch of the foot. It is embedded in the plantar fascia which is a band of tissue that extends from the heel to the toes along the bottom of the foot. There can be multiple plantar fibromas in the feet at the same time. There are no known causes for this condition. If you have a plantar fibroma, there will be a bump in the arch of your foot that cannot be missed. Any associated pain is most often due to a shoe rubbing against the nodule. Non-surgical options, such as steroid injections, physical therapy, and orthotics should be tried first. Surgery is a last resort and is the only thing that will remove a plantar fibroma entirely. Consult with a podiatrist for a proper diagnosis and to determine the treatment regimen that is right for you.
What Causes a Plantar Fibroma?
While there are no specific causes identified, a plantar fibroma can possibly come from genetic predisposition or the formation of scar tissue that forms from healing the tears in the plantar fascia.
What Are the Symptoms of a Plantar Fibroma?
There will be a noticeable lump in the arch of the foot that may or may not cause pain. If pain is felt, it is typically because a shoe is rubbing up against the lump or when walking or standing barefoot.
Treatment and Prevention
A plantar fibroma will not disappear without treatment, but it can get smaller and be a non-issue. If pain persists, a podiatrist examines the foot and when the arch of the foot is pressed, pain can be felt down to the toes. An MRI or biopsy might be performed to help diagnose or evaluate the plantar fibroma. The following non-surgical options are generally enough to reduce the size and pain of these nodules:
Surgery is considered if the mass increases in size and the patient continues to feel pain after non-surgical methods are tried.
If you have any questions, please feel free to contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A plantar fibroma is a knot in the arch of the foot. It can cause pain when repeated pressure is applied by walking barefoot or wearing tight shoes. While plantar fibromas can appear in anyone, men who are middle-aged or older are said to be more susceptible. The main symptom of a plantar fibroma is a firm lump on the arch of the foot. If there is pain, it can be intensified by putting pressure on the nodule. The lump can stay one size or grow larger. You may have one or more fibromas in the feet and there tends to be a high incidence of recurring plantar fibromas. Generally, a plantar fibroma can be treated without surgery. Treatment might include steroid injections to help shrink the lump, orthotics to help redistribute weight away from the nodule, plantar fascia stretching, or physical therapy to help use anti-inflammatory medication on the lump. If a lump grows larger or more painful, a podiatrist can be consulted to confirm the diagnosis. The doctor will palpate the lump and this may cause pain that can be felt all the way to the toes. An X-ray, MRI, or biopsy might be done if further evaluation is necessary. A lump in the arch of the foot might be something other than a plantar fibroma, such as cysts, nerve or fatty tumors, swollen tendons, or an infection in the foot. It is important to see a podiatrist for proper diagnosis and treatment of plantar fibromas.