In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.
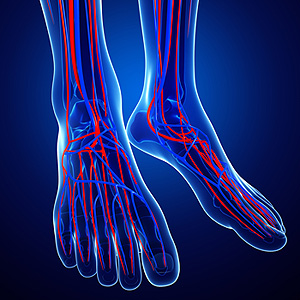 Peripheral artery disease, also known as PAD, is a condition that results in poor circulation to the lower limbs. Typical symptoms of PAD include leg pain or muscle cramps when walking, numbness, weakness, or coldness in your legs. An ankle brachial index is a quick, noninvasive, and painless test used to screen for PAD. The measurements can highlight any potential problems, like blockages or partial blockages in blood flow to your extremities.To do this test, a doctor simply takes your blood pressure at your arms and at your ankles and compares the numbers to come up with a numerical ratio that represents your risk of having or developing PAD. While anyone can get the ankle brachial index test, people who have pre-existing risk factors for developing PAD are especially encouraged to undergo this screening. Risk factors include a history of smoking, high blood pressure, high cholesterol, diabetes, and atherosclerosis. For more information about the ankle brachial index and other tests for PAD, speak with a podiatrist today.
Peripheral artery disease, also known as PAD, is a condition that results in poor circulation to the lower limbs. Typical symptoms of PAD include leg pain or muscle cramps when walking, numbness, weakness, or coldness in your legs. An ankle brachial index is a quick, noninvasive, and painless test used to screen for PAD. The measurements can highlight any potential problems, like blockages or partial blockages in blood flow to your extremities.To do this test, a doctor simply takes your blood pressure at your arms and at your ankles and compares the numbers to come up with a numerical ratio that represents your risk of having or developing PAD. While anyone can get the ankle brachial index test, people who have pre-existing risk factors for developing PAD are especially encouraged to undergo this screening. Risk factors include a history of smoking, high blood pressure, high cholesterol, diabetes, and atherosclerosis. For more information about the ankle brachial index and other tests for PAD, speak with a podiatrist today.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with one of our podiatrists from Jill Einhorn, DPM and James Einhorn, DPM. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
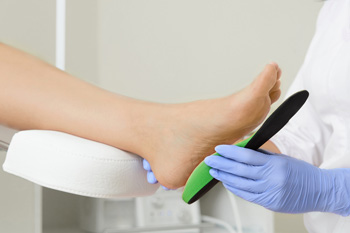 Orthotics are devices used to help correct, support, and align different ailments, injuries, or deformities the body may be experiencing. Orthotics are often a common method of treatment in the world of podiatry, acting as a supportive and corrective device for a number of different conditions. Most orthotics come prefabricated, but a podiatrist can take the time to have a fitting with their patients, making sure it’s custom molded for their needs. It’s essential to get a proper fitting orthotic device, that way you can prevent any additional issues from developing. Some common foot conditions orthotics have been known to help are bunions, plantar fasciitis, heel spurs, and neuromas. If you have a foot condition you believe could benefit from the aid of an orthotic device, please consult with a podiatrist for their professional advice and a proper fitting consultation.
Orthotics are devices used to help correct, support, and align different ailments, injuries, or deformities the body may be experiencing. Orthotics are often a common method of treatment in the world of podiatry, acting as a supportive and corrective device for a number of different conditions. Most orthotics come prefabricated, but a podiatrist can take the time to have a fitting with their patients, making sure it’s custom molded for their needs. It’s essential to get a proper fitting orthotic device, that way you can prevent any additional issues from developing. Some common foot conditions orthotics have been known to help are bunions, plantar fasciitis, heel spurs, and neuromas. If you have a foot condition you believe could benefit from the aid of an orthotic device, please consult with a podiatrist for their professional advice and a proper fitting consultation.
If you are having discomfort in your feet and would like to try orthotics, contact one of our podiatrists from Jill Einhorn, DPM and James Einhorn, DPM. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Are Orthotics?
Orthotics are inserts you can place into your shoes to help with a variety of foot problems such as flat feet or foot pain. Orthotics provide relief and comfort for minor foot and heel pain but can’t correct serious biomechanical problems in your feet.
Over-the-Counter Inserts
Orthotics come in a wide variety of over-the-counter inserts that are used to treat foot pain, heel pain, and minor problems. For example, arch supports can be inserted into your shoes to help correct overarched or flat feet, while gel insoles are often used because they provide comfort and relief from foot and heel pain by alleviating pressure.
Prescription Orthotics
If over-the-counter inserts don’t work for you or if you have a more severe foot concern, it is possible to have your podiatrist prescribe custom orthotics. These high-quality inserts are designed to treat problems such as abnormal motion, plantar fasciitis, and severe forms of heel pain. They can even be used to help patients suffering from diabetes by treating foot ulcers and painful calluses and are usually molded to your feet individually, which allows them to provide full support and comfort.
If you are experiencing minor to severe foot or heel pain, it’s recommended to speak with your podiatrist about the possibilities of using orthotics. A podiatrist can determine which type of orthotic is right for you and allow you to take the first steps towards being pain-free.
If you have any questions please contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Orthotics are shoe inserts that are meant to correct an irregular walking gait or provide cushioning to the feet. Orthotics come in a variety of different models and sizes, including over-the-counter and customizable variants. Customizable orthotics can be shaped and contoured to fit inside a specific shoe and are typically prescribed through a podiatrist who specializes in customized footwear and orthotics design and management.
Orthotics are beneficial because they can help prevent injuries from occurring and provide cushioning to keep pain levels down to a minimum. They also allow for the correct positioning of the feet. Orthotics can act as shock absorbers to help remove pressure from the foot and ankle. Therefore, orthotics can make bodily movements, such as walking and running, become more comfortable as well as help prevent the development of certain foot conditions.
Orthotics alleviate pain and make the foot more comfortable by slightly altering the angle at which the foot strikes the ground surface, therefore controlling the movement of the foot and ankle. Orthotics come in different variants and can be made of various materials. To determine what type of orthotic is most suited to your feet and your needs, it is best to consult your podiatrist. He or she will be able to recommend a type of orthotic that can help improve your foot function or prescribe a custom orthotic to best fit your feet.
 Morton’s neuroma can occur when nerve tissue swells or grows abnormally, causing damage to the nerves. Morton’s neuroma specifically affects the intermetatarsal plantar nerve found in the foot. Some symptoms of this condition may include a burning sensation in the ball of your foot and tingling, or a numbing feeling in your toes. The most popular symptom related to Morton’s neuroma is feeling as if a pebble is stuck in your shoe. For a proper diagnosis, please consult with a podiatrist if you believe you’re experiencing symptoms of Morton’s neuroma.
Morton’s neuroma can occur when nerve tissue swells or grows abnormally, causing damage to the nerves. Morton’s neuroma specifically affects the intermetatarsal plantar nerve found in the foot. Some symptoms of this condition may include a burning sensation in the ball of your foot and tingling, or a numbing feeling in your toes. The most popular symptom related to Morton’s neuroma is feeling as if a pebble is stuck in your shoe. For a proper diagnosis, please consult with a podiatrist if you believe you’re experiencing symptoms of Morton’s neuroma.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact one of our podiatrists of Jill Einhorn, DPM and James Einhorn, DPM. Our doctors will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Morton's NeuromaA neuroma is a thickening of nerve tissue and can develop throughout the body. In the foot, the most common neuroma is a Morton’s neuroma; this typically forms between the third and fourth toes. The thickening of the nerve is typically caused by compression and irritation of the nerve; this thickening can in turn cause enlargement and, in some cases, nerve damage.
Neuromas can be caused by anything that causes compression or irritation of the nerve. A common cause is wearing shoes with tapered toe boxes or high heels that force the toes into the toe boxes. Physical activities that involve repeated pressure to the foot, such as running or basketball, can also create neuromas. Those with foot deformities, such as bunions, hammertoes, or flatfeet, are more likely to develop the condition.
Symptoms of Morton’s neuroma include tingling, burning, numbness, pain, and the feeling that either something is inside the ball of the foot or that something in one’s shoe or sock is bunched up. Symptoms typically begin gradually and can even go away temporarily by removing one’s shoes or massaging the foot. An increase in the intensity of symptoms correlates with the increasing growth of the neuroma.
Treatment for Morton’s neuroma can vary between patients and the severity of the condition. For mild to moderate cases, padding, icing, orthotics, activity modifications, shoe modifications, medications, and injection therapy may be suggested or prescribed. Patients who have not responded successfully to less invasive treatments may require surgery to properly treat their condition. The severity of your condition will determine the procedure performed and the length of recovery afterwards.
 Sever’s disease, also known as calcaneal apophysitis, is not a disease at all, but rather an overuse injury. This condition affects the growth plate of the heel bone and is therefore most common in children and teenagers who are still rapidly growing. Sever’s disease causes inflammation in the heel, stiffness in the foot, and pain when standing, walking, running or jumping that usually improves with rest. Children who are involved in sports are the most at risk for developing Sever’s disease because they put frequent, repetitive pressure on the heel. Other risk factors for developing this condition include wearing ill-fitting shoes, having flat arches or pronated feet, and obesity. If your child is experiencing heel pain and stiffness, it is recommended that you take them to a podiatrist for treatment.
Sever’s disease, also known as calcaneal apophysitis, is not a disease at all, but rather an overuse injury. This condition affects the growth plate of the heel bone and is therefore most common in children and teenagers who are still rapidly growing. Sever’s disease causes inflammation in the heel, stiffness in the foot, and pain when standing, walking, running or jumping that usually improves with rest. Children who are involved in sports are the most at risk for developing Sever’s disease because they put frequent, repetitive pressure on the heel. Other risk factors for developing this condition include wearing ill-fitting shoes, having flat arches or pronated feet, and obesity. If your child is experiencing heel pain and stiffness, it is recommended that you take them to a podiatrist for treatment.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see one of our podiatrists from Jill Einhorn, DPM and James Einhorn, DPM. Our doctors can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.
Sever’s disease, also known as calcaneal apophysitis is a common bone disorder that occurs during childhood. The disease is defined as an inflammation of the growth plate in the heel. When a child has a growth spurt, his heel bone grows faster than the muscles, tendons, and ligaments in his leg. This disease is a result of overuse. The people who are most likely to be affected by this disease are children who are in a growth spurt, especially boys who are from the ages of 5 to 13 years old. 60% of children with Sever’s disease have both heels involved.
Symptoms of this disease are heel pain that intensifies during running and jumping activities. The pain is typically localized to the posterior part of the heel. Symptoms may be severe, and they can easily interfere with daily activities. Children who play soccer, baseball, and basketball are more likely to develop Sever’s disease.
Your doctor will diagnose your child based on his or her symptoms, x-rays are generally not helpful in diagnosing this disease. Your doctor may examine both heels and ask your child questions about his or her activity level in sports. Your doctor may then use the squeeze test on your child’s heel to see if there is any pain. Nevertheless, some doctors might still use x-rays to rule out any other issues such as fractures, infections, and tumors.
Sever’s disease can be prevented by maintaining good flexibility while your child is growing. Another prevention method is to wear good-quality shoes that have firm support and a shock-absorbent sole. Sever’s disease can be treated by ceasing any activity that causes heel pain. You should apply ice to the injured heel for 20 minutes 3 times a day. Additionally, orthotics should be used for children who have high arches, flat feet, or bowed legs.
If you suspect your child has Sever’s disease, you should make an appointment with your podiatrist to have his or her foot examined. Your doctor may recommend nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen to relieve pain. In more severe cases, your child may need a cast to rest his or her heel. Fortunately, Sever’s disease does not cause long-term foot problems. After treatment, your child should start to feel better within two weeks to two months.
 A stress fracture is a small crack in a bone that can cause swelling and pain that increases over time. Stress fractures in the feet and ankles are notoriously common among runners and athletes who participate in sports that require frequent running, such as soccer. A stress fracture can take weeks or even months to heal, often requiring a walking boot, brace, or crutches to keep weight off of the affected foot. This can sideline an athlete from both their sport and activities of daily living. Fortunately, there are things that you can do that might prevent these injuries. When running, increase the amount of miles that you run slowly, as running too much too soon puts enormous strain on your muscles and bones. You may want to take days off from your sport or exercise routine to rest your feet. It is also recommended that you get enough sleep, eat a balanced diet, and avoid processed sugars, which can increase inflammation in the body. If you suspect you may have a stress fracture or want to learn more about what you can do to prevent this injury, consult with a podiatrist today.
A stress fracture is a small crack in a bone that can cause swelling and pain that increases over time. Stress fractures in the feet and ankles are notoriously common among runners and athletes who participate in sports that require frequent running, such as soccer. A stress fracture can take weeks or even months to heal, often requiring a walking boot, brace, or crutches to keep weight off of the affected foot. This can sideline an athlete from both their sport and activities of daily living. Fortunately, there are things that you can do that might prevent these injuries. When running, increase the amount of miles that you run slowly, as running too much too soon puts enormous strain on your muscles and bones. You may want to take days off from your sport or exercise routine to rest your feet. It is also recommended that you get enough sleep, eat a balanced diet, and avoid processed sugars, which can increase inflammation in the body. If you suspect you may have a stress fracture or want to learn more about what you can do to prevent this injury, consult with a podiatrist today.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact one of our podiatrists from Jill Einhorn, DPM and James Einhorn, DPM. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Brooklyn and Astoria, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.